Last week I had surgery to reconstruct my pelvic floor. And, being very much me, I went into full research mode.
Before this, I honestly wasn’t very aware that this kind of surgery even existed — and I suspect many other women are the same, unless they’ve supported a loved one through it or experienced pelvic floor issues themselves. I wanted to properly understand what had been done to my body, why it was necessary, and what that meant for my recovery.
One thing that really helped was learning the difference between a posterior colporrhaphy and a colpoperineorrhaphy. Understanding this has helped me make sense of my symptoms, my healing, and why recovery feels the way it does. I’m sharing it here in the hope it helps another woman feel a little less confused and a little more informed.
What is a posterior prolapse repair?
A standard posterior prolapse repair is often called a posterior colporrhaphy.
This surgery focuses on the back wall of the vagina, where the rectum can push or bulge forward. This bulge is known as a rectocele.
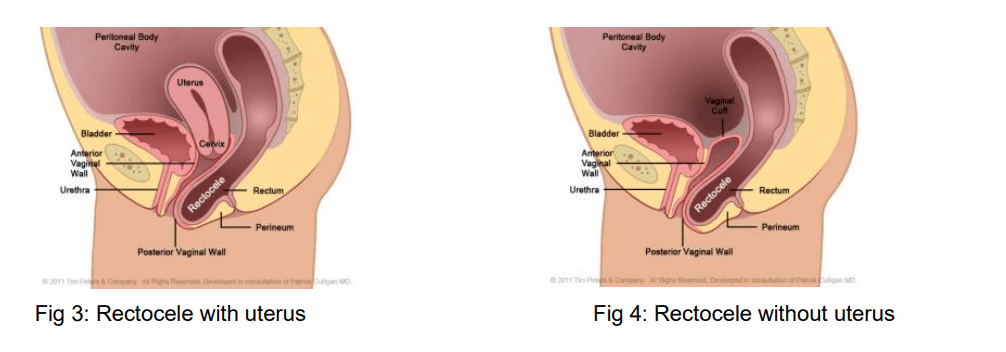
The aim of a posterior colporrhaphy is to:
- Strengthen and reinforce the vaginal wall
- Reduce the bulge created by the rectum
- Improve symptoms related to bowel emptying and pressure
For some women, particularly those with milder prolapse or fewer symptoms, this type of repair can be enough.
What is a colpoperineorrhaphy?
A colpoperineorrhaphy is a more extensive repair.
It includes:
- A posterior vaginal wall repair
- Reconstruction of the perineum, the tissue and muscles between the vagina and anus
The perineum plays a crucial role in pelvic stability, bowel support, and continence. Over time (and often after childbirth, surgery, menopause, or connective tissue issues), this area can become weakened or stretched.
This surgery doesn’t just address the visible bulge; it works on the structural foundation underneath. In other words, it’s not only repairing the wall, but also rebuilding the support system that holds everything in place.
For women with more advanced prolapse, ongoing bowel symptoms, or perineal damage, this deeper reconstruction can be necessary.
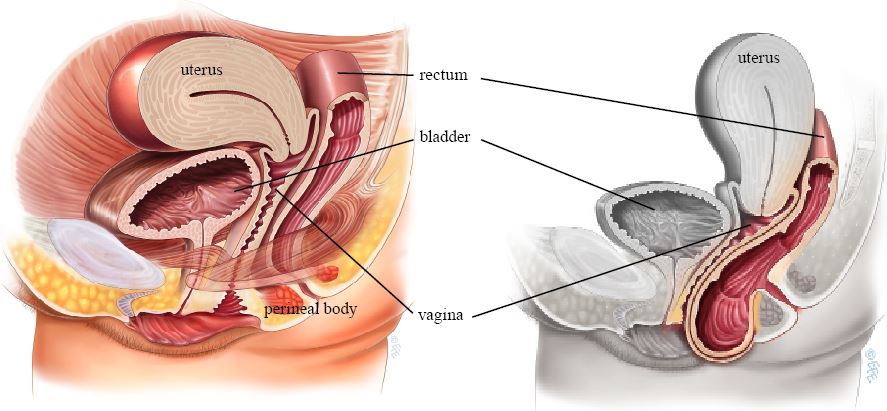
Source:yourpelvicfloor.org
Symptoms: What Might You Notice With a Posterior Prolapse?
Posterior prolapse symptoms can be subtle at first, which is why many women live with them for years before realising what’s going on.
Common symptoms include:
- A feeling of pressure, heaviness, or fullness in the vagina
- The sensation of something bulging or sitting low
- Difficulty emptying the bowels fully
- Needing to strain despite soft stools
- A feeling of blockage or obstruction when trying to poo
- Needing to change position or apply pressure to help bowel emptying
- Lower back or pelvic discomfort, especially after standing or walking
Symptoms that worsen as the day goes on
Some women describe it as feeling like things are “falling down” or “out of alignment,” while others simply know that something doesn’t feel right.
Why Understanding the Surgery Matters for Recovery
Knowing whether you’ve had a posterior colporrhaphy or a colpoperineorrhaphy can really help you make sense of recovery.
A more extensive repair often means:
- A stronger sense of tightness or pulling during healing
- More emphasis on rest, lying down, and pressure reduction
- Slower return to normal movement and activity
A longer timeline for tissues to fully settle
Healing isn’t just about the surface stitches. it’s about deep muscles and connective tissue, relearning how to support you again. That takes time, patience, and a lot of kindness toward your body.
Why talking about this matters
Pelvic floor surgery isn’t something we talk about openly enough, yet so many women are quietly living with prolapse symptoms without understanding what’s happening or knowing that help exists.
Learning the language and the differences between procedures has been empowering for me, not because it makes recovery quicker, but because it makes it less frightening and less lonely.
If you’re navigating this yourself, please know: you’re not broken, you haven’t failed, and you’re certainly not alone. Your body has carried you through a lot, and now it’s time to let it heal.
I will share my healing journey with you.
Love & healing hugs

Blog Series
Sitting With Vulnerability: A Life Update
What unsettles me isn’t the surgery itself; it’s the vulnerability.
Understanding Posterior Prolapse Repair & Colpoperineorrhaphy
Making sense of the surgery and healing
Post Colpoperineorrhaphy Surgery Recovery: Embracing Rest and Healing
Talking matters, even when the subject isn’t sexy. Especially when it isn’t.
Supporting Your Bowels Without Strain After a Colpoperineorrhaphy
“How do I eat enough fibre without making things worse?”
First Week Post Op Colpoperineorrhaphy
This feels like a milestone worth marking.
Further reading:
Royal College of Obstetricians and Gynaecologists Recovering Well leaflet at
https://www.rcog.org.uk/globalassets/documents/patients/patientinformationleaflets/recovering-well/pelvic-floor-repair-operation.pdf
Royal College of Obstetricians and Gynaecologists patient information
leaflet – Pelvic organ prolapse at
https://www.rcog.org.uk/globalassets/documents/patients/patientinformationleaflets/Gynaecology/pi-pelvic-organ-prolapse.pdf
Leave a comment